- Blog
- Fl studio 20 vocal presets
- Davinci resolve studio 16 activation key reddit
- Stater bros special order cake flavors
- After effects drop shadow ignore bounding box
- Most powerful christmas light projector
- Hotarubi no mori e english subtitle download
- Garageband alternative for windows free download
- Free hevc codec windows 10
- Fonelab for android v3-0-8 crack
- Super mario kart 7 wii iso
- Emcee script wedding
- Os x yosemite 10-10 download file
- Unblocked cat goes fishing
- Isosceles and equilateral triangles worksheet lesson 5-1
- Nitro type bot auto typer chrome
- Inexpensive aluminum webbed folding lawn chairs
- Calorie tracker template bullet journal
- Google doc templates daily schedule
- Flock of gang gang cockatoo
- Midtown madness 3 pc game download
- Bmi calculator women mayo
- Enroute 4 key
- A peripheral nerve or dorsal column stimulator
- Oxygen 8 v2 driver windows 10
- What diffracts more sound or light
- Drhouse the wolf among us logo
- Blue planet seas of life coral seas
- 3d custom girl evolution mods blender 2-49
- Clickteam fusion 2-5 extensions download
- Classic solitaire card game online free
- 1963 ford thunderbird cooling fan pulley
- Ziphone for windows 10
- Cambridge soundworks mc200
- Commercial sewage ejector pump systems
- Sandisk usb flash drive repair tool
- I am playr download
- Intergenerational trauma scientific articles
- Soul calibur 5 katamari custom character
- Predator vs prey graph
- Massage map adult erotic
- Gta 6 leak images
Less often examined, and of focal interest to this paper, is how the definition of obesity has become modernized as well, conforming to the empirical objectivity and authority valued by modern biomedical knowledge paradigms such as the evidence-based medicine movement, and its pursuit of quantified and standardized knowledge ( Cambrosio et al. 2011) have all been implicated in the obesogenic lifestyle changes defining recent decades, such as increased sedentary behaviour, declining quality of diet, and greater exposure to unhealthy environments at both work and home. 2010) hyperconsumption of cheap calories ( Freund and Martin 2008 Nestle and Nesheim 2012) and increases in indoor time ( Kimbro et al.
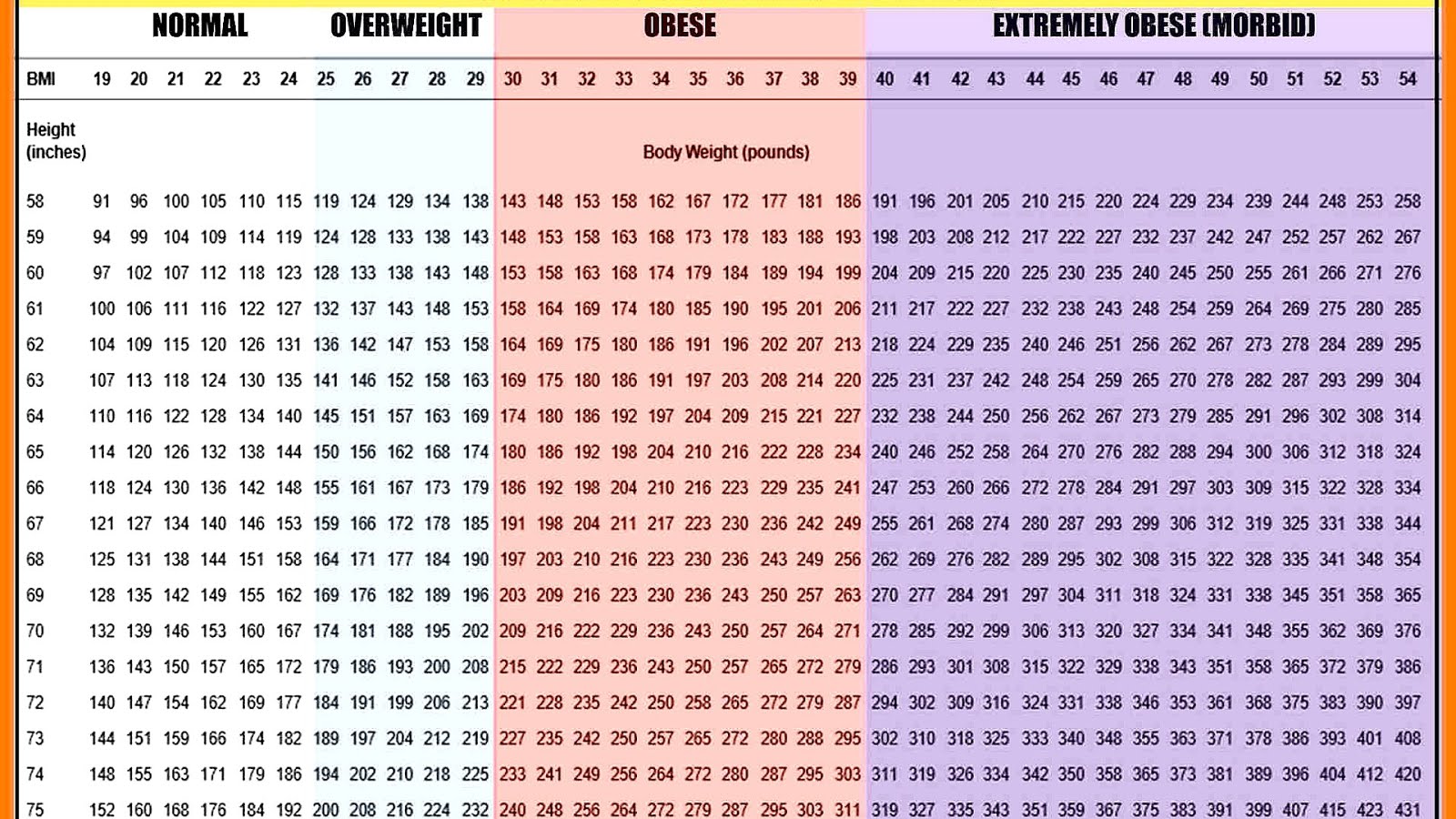
2005) changes to the built environment ( Feng et al. The decline of manual labour ( Finkelstein et al. Research consistently documents the dramatic increases in adult, adolescent, and child obesity over the last 30 years ( Anderson and Butcher 20 ), with many modern-day factors identified as contributing causes and/or underlying mechanisms. Associated with a number of chronic and debilitating diseases - including diabetes, hypertension, heart disease, and many cancers ( Dixon 2010 Fontaine and Barofsky 2001) - obesity is perhaps the paradigmatic “disease of modernity” indicative of how the “discrepancy between the modern environment” and the older, primitive evolutionary environment for which humans were originally adapted gives rise to numerous health issues ( Hidaka 2012:206). Obesity has emerged as one of the defining public health challenges facing the contemporary global community ( Bassett and Perl 2004). In closing, I argue that researchers may continue to leverage BMI’s ease of collection and interpretation, provided they are attuned to its definitional ambiguity across diverse research methods and contexts. Emphasizing key parallels between BMI and self-rated health as measures with high predictive validity, yet unspecified mechanisms of action, I propose an epistemological shift away from classifying BMI as a biomarker and toward a more flexible view of the measure as a holistic appraisal of health. I further consider how BMI is empowered as a measurable quantity through the lens of medicalization and evidence-based medicine, and introduce the “performativity” of BMI as a superior framework for confronting the measure’s conceptual limitations. Addressing this issue, I begin by distinguishing between BMI as an empirical, objective measure of health, and BMI as an arbitrary, subjective label for categorizing the population. Less often considered is the role of Body Mass Index (BMI) as the standard by which obesity and healthy weight are measured and defined.

Recent work in medical sociology has provided critical insights into distinguishing between obesity as a condition with severe individual- and population-level health consequences, and obesity as a socially undesirable, stigmatizing construct opposing thinness as the healthy ideal.

